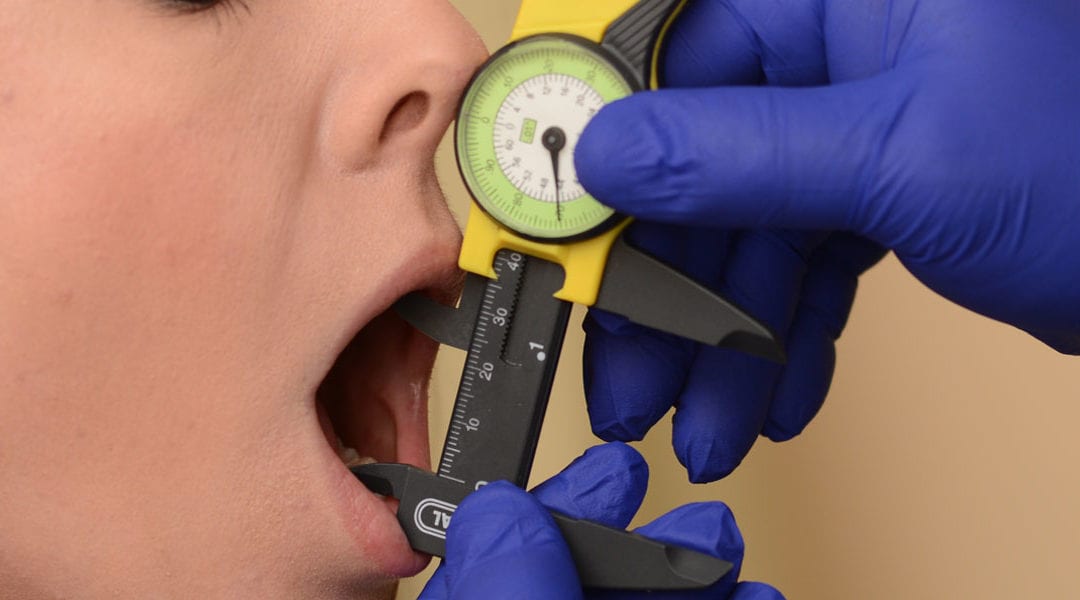
Headaches are common among the general population and positively associated with several musculoskeletal disorders including temporomandibular disorders (TMD). The objective of this study was to explore the presence of possible confounders of the association between TMD and headaches. Several subtypes of headaches were classified: self-reported headache, migraine, Tension-Type Headaches and secondary headache attributed to TMD. The presence of Temporomandibular Disorders (TMD) was subdivided into two subtypes: painful TMD and function-related TMD. (I will discuss the epidemiology of headaches shortly.) Of the patients who were referred to the TMD and Orofacial Pain Clinic (N=205}, 66.8% experienced headaches. From the subsample of patients with a painful TMD (n=59), the prevalence of self-reported headaches increased to 81.4%. There was a significant association between self-reported headache and both painful TMD and function-related TMD, as well as between probable migraine and painful TMD.
The Association Between Headaches and Temporomandibular Disorders Is Confounded by Bruxism and Somatic Complaints: HA van der Meer et al. Clin J Pain. 2016 Dec 19.
Globally, it has been estimated that the prevalence among adults of current headache disorder (symptomatic at least once within the last year) is about 50%. Half to three quarters of adults aged 18–65 years in the world have had a headache in the last year. Among those individuals, 30% or more have reported a migraine. Headache on 15 or more days every month affects 1.7–4% of the world’s adult population. Despite regional variations, headache disorders are a worldwide problem, affecting people of all ages, races, income levels and geographical areas. Not only is headache painful, but it is also disabling. In the Global Burden of Disease Study, updated in 2013, migraine on its own was found to be the sixth highest cause worldwide of years lost due to disability (YLD). Headache disorders collectively were third highest.
Types of headache disorders
Migraine, tension-type headache and medication-overuse headache are of public health importance since they are responsible for high population levels of disability and ill-health.
Migraine
- A primary headache disorder.
- Migraine most often begins at puberty and most affects those aged between 35 and 45 years.
- It is more common in women, usually by a factor of about 2:1, because of hormonal influences.
- It is caused by the activation of a mechanism deep in the brain that leads to release of pain-producing inflammatory substances around the nerves and blood vessels of the head.
- Migraine is recurrent, often life-long, and characterized by recurring attacks.
- Attacks typically include:
- headache, which is:
- of moderate or severe intensity
- one-sided
- pulsating in quality
- aggravated by routine physical activity
- with duration of hours to 2-3 days
- nausea (the most characteristic associated feature);
- attack frequency is anywhere between once a year and once a week; and
- in children, attacks tend to be of shorter duration and abdominal symptoms more prominent.
- headache, which is:
Tension-type headache (TTH)
- TTH is the most common primary headache disorder.
- Episodic TTH, occurring on fewer than 15 days per month, is reported by more than 70% of some populations.
- Chronic TTH, occurring on more than 15 days per month, affects 1-3% of adults.
- TTH often begins during the teenage years, affecting three women to every two men.
- Its mechanism may be stress-related or associated with musculoskeletal problems in the neck.
- Episodic TTH attacks usually last a few hours, but can persist for several days.
- Chronic TTH can be unremitting and is much more disabling than episodic TTH.
- This headache is described as pressure or tightness, often like a band around the head, sometimes spreading into or from the neck.
Cervicogenic Headache
- Neck pain and tenderness are common symptoms present in many headache disorders.
- When cervical dysfunction or degenerative changes cause headache it is referred to as cervicogenic headache.
- Cervicogenic headache prevalence is estimated at .5% to 4%, but may be as high as 20% of patients presenting with severe chronic headaches.
- The mean age of patients with this condition is 43 years.
- The condition is more common in women.
- Pain is referred from a source in the neck and felt in one or more regions of the head and/or face.
Cluster Headache (CH)
- A primary headache disorder.
- CH is relatively uncommon affecting fewer than 1 in 1000 adults, affecting six men to each woman.
- Most people developing CH are in their 20s or older.
- It is characterized by frequently recurring (up to several times a day), brief but extremely severe headache, usually focused in or around one eye, with tearing and redness of the eye, the nose runs or is blocked on the affected side and the eyelid may droop.
- CH has episodic and chronic forms.
Medication-overuse headache (MOH)
- MOH is caused by chronic and excessive use of medication to treat headache.
- MOH is the most common secondary headache disorder.
- It may affect up to 5% of some populations, women more than men.
- MOH occurs by definition on more days than not, is oppressive, persistent and often at its worst on awakening.
Barriers to effective care
Lack of knowledge among health-care providers is the principal clinical barrier. Worldwide, on average, only 4 hours of undergraduate medical education are dedicated to instruction on headache disorders. A large number of people with headache disorders are not diagnosed and treated: worldwide only 40% of those with migraine or TTH are professionally diagnosed, and only 10% of those with MOH.
Poor awareness extends to the general public. Headache disorders are not perceived by the public as serious since they are mostly episodic, do not cause death, and are not contagious. The low consultation rates in developed countries may indicate that many affected people are unaware that effective treatments exist. Half of people with headache disorders are estimated to be self-treating.
Treatment
Appropriate treatment of headache disorders requires training of health professionals, accurate diagnosis and recognition of the conditions. Seeing a physical therapist that is skilled and has certifications in TMD, Cervical spine and Headache disorders will certainly improve your chances of finding relief or at least life management tools. Each of our locations at Freedom Physical Therapy Services has physical therapists with these skills and credentials. I also encourage you to check out this link to a small group of us physical therapists throughout the USA that have the credentials of CCTT, Certified Cervical and Temporomandibular Therapeutics, http://www.ptbcct.org/ . I have also done a blog on Chronic overlapping pain conditions https://freedompt.com/nipping-chronic-pain-in-the-bud/ . I have personally found many of my TMD and headache patients have several musculoskeletal issues going on at once, and if all are treated effectively, I find our patients have far better outcomes. I always say to patients, the more “fires” we can “put out” that your body is experiencing, the better overall reduction in pain and improvement in function. As with many other conditions appropriate treatment with cost-effective medications, simple lifestyle modifications, and patient education are of great benefit.
So why suffer needlessly with your headaches, work hard to find health care professionals that can offer you a comprehensive view of head, neck and face pain disorders!
Enjoy More Freedom!
Michael Karegeannes
Owner Freedom PT Services